Document Type : Systematic Review
Authors
1
Department of Health Information Technology, Ferdows School of Health and Allied Medical Sciences, Birjand University of Medical Sciences, Birjand, Iran
2
Department of Health Information Management, School of Allied Medical Sciences, Tehran University of Medical Sciences, Tehran, Iran
3
“Student Research Committee” and “Department of Health Information Technology, School of Paramedical Sciences”, Mashhad University of Medical Sciences, Mashhad, Iran
4
Department of Statistics and Information Technology, Gonabad University of Medical Sciences, Gonabad, Iran
5
Department of Health Information Technology, Army University of Medical Sciences, Tehran, Iran
Abstract
Aims: Electronic health can lead to health preservation and promotion using information and communication technologies to receive and record accurate data, appropriate storage, and retrieval, as well as the health information management approach. The present systematic review aimed to assess the E-health application during the COVID-19.
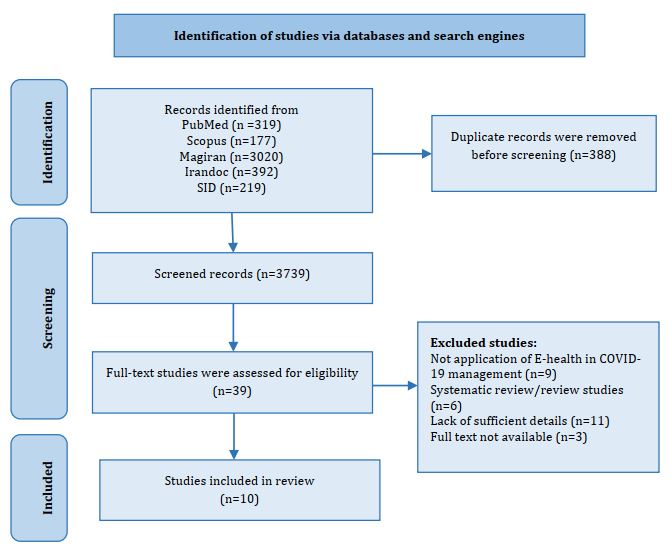
Information & Methods: The present systematic review was done based on PRISMA protocols. The study data were retrieved using the E-health and COVID-19 keywords in the related studies from August 4, 2021, in PubMed, Scopus, Magiran, and Sid databases. Moreover, the inclusion criteria were original research studies that used E-health to manage patients with COVID-19.
Findings: A total of 10 articles were included in the study, 40% of which focused on the impact of E-health on reducing fear and anxiety caused by COVID-19, 30% on the E-health in early diagnosis and progression of the disease, 10% on the E-health application in the field of prevention, 10% on E-health in the field of disease control, and 10% on E-health for quick investigations of the disease process and access new medical information. The used technologies included virtual training through WhatsApp video calling, Instagram, iGap and Telegram voice and text messaging, artificial intelligence, and data mining techniques.
Conclusion: E-health tools played a prominent role during the COVID-19 in the prevention, diagnosis, control, and fear reduction of coronavirus disease. Various practical strategies such as financing, implementation and legal requirements can be considered to effectively use the capabilities of eHealth tools in disease management.
Keywords
Subjects