Volume 10, Issue 1 (2022)
Health Educ Health Promot 2022, 10(1): 1-7 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Zareban I, Rahmani A, Allahqoli L, Ghanei Gheshlagh R, Hashemian M, Khayyati F, et al . Effect of Education Based on Trans-Theoretical Model in Social Media on Students with Gingivitis; a Randomized Controlled Trial. Health Educ Health Promot 2022; 10 (1) :1-7
URL: http://hehp.modares.ac.ir/article-5-50157-en.html
URL: http://hehp.modares.ac.ir/article-5-50157-en.html
I. Zareban1, A. Rahmani2, L. Allahqoli3, R. Ghanei Gheshlagh4, M. Hashemian *5, F. Khayyati6, S. Wai-chi Chan7, T. Volken8, B. Nemat9
1- Health Promotion Research Centre, Zahedan University of medical sciences, Zahedan, Iran
2- Nursing and Midwifery Care Research Center, School of Nursing and Midwifery, Tehran University of Medical Sciences, Tehran, Iran
3- Department of Public Health, Iran University of Medical Sciences, Tehran, Iran
4- Spiritual Health Research Center, Research Institute for Health Development, Kurdistan University of Medical Sciences, Sanandaj, Iran
5- Department of Public Health & Health Education, Faculty of Health, Sabzevar University of Medical Sciences, Sabzevar, Iran
6- Social Determinants of Health Research Center, Research Institute for Health Development, Kurdistan University of Medical Sciences, Sanandaj, Iran
7- Department of Nursing and Midwifery, Faculty of Health and Medicine, University of Newcastle, Australia
8- School of Health Professions, Zurich University of Applied Sciences, Winterthur, Switzerland
9- Health Network of Sanandaj, Kurdistan University of Medical Sciences, Sanandaj, Iran
2- Nursing and Midwifery Care Research Center, School of Nursing and Midwifery, Tehran University of Medical Sciences, Tehran, Iran
3- Department of Public Health, Iran University of Medical Sciences, Tehran, Iran
4- Spiritual Health Research Center, Research Institute for Health Development, Kurdistan University of Medical Sciences, Sanandaj, Iran
5- Department of Public Health & Health Education, Faculty of Health, Sabzevar University of Medical Sciences, Sabzevar, Iran
6- Social Determinants of Health Research Center, Research Institute for Health Development, Kurdistan University of Medical Sciences, Sanandaj, Iran
7- Department of Nursing and Midwifery, Faculty of Health and Medicine, University of Newcastle, Australia
8- School of Health Professions, Zurich University of Applied Sciences, Winterthur, Switzerland
9- Health Network of Sanandaj, Kurdistan University of Medical Sciences, Sanandaj, Iran
Keywords: Oral Health [MeSH], Education [MeSH], Social Media [MeSH], Students [MeSH], Gingivitis [MeSH], Behavior [MeSH]
Full-Text [PDF 492 kb]
(1114 Downloads)
| Abstract (HTML) (1897 Views)
Table 1) Key for determining the stage of change based on responses to the stages of change instrument [17]
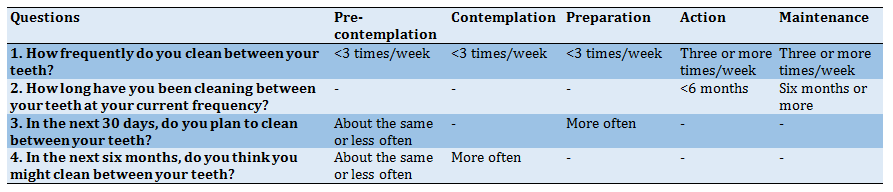
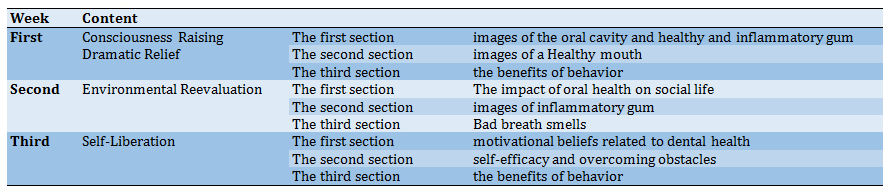
Table 2) Content of 3 weeks of intervention based on trans-theoretical model
Full-Text: (309 Views)
Introduction
Oral health is a state of tooth structure and tissue linked to physical, psychological, and social well-being. Oral health co-determines if and how people will be able to talk, eat and socialize [1-3]. Despite the importance of oral health, more than 99% of people worldwide suffer from oral diseases [4], negatively impacting their communication abilities, daily performance, and poor voice quality. They may also suffer from pain and anxiety [5-7]. Worldwide, dental caries has increased significantly, especially in adolescents [8]. The World Health Organization (WHO) has called for global initiatives to reduce the burden of oral diseases in adolescents [9].
Located in the eastern Mediterranean region [10], Iran is one of the youngest countries in the world which 50% are under the age of 30 years [11]. The incidence of dental caries in Iranian students is over 90% [12], and one-third of them suffer from gingivitis [13]. These figures indicated the necessity of educational programs which aim to maintain and promote oral health in students [14, 15].
Many education programs developed based on behavioral change models, such as the trans-theoretical model, have shown high efficacy in preventing oral diseases [1]. Although some studies have evaluated the application of the trans-theoretical model in promoting Dental Cleaning Behavior (DCB) [1, 16, 17], the researchers did not have access to research that assessed the effects of a health education program supported by the trans-theoretical model and delivered via social media app.
The Trans-Theoretical Model (TTM) is a purposeful behavioral change model. It is a systematic study of individuals' behavioral changes and describes how people move dynamically through five different stages of behavioral changes. The four core constructs of TTM are stages of change (Precontemplation, Contemplation, Preparation, Action, Maintenance), self-efficacy, decisional balance, and change processes. The TTM holds that people begin to perceive more benefits than disadvantages from adopting positive behavior changes as they move through the later stages [18].
Social media is one of the recent revolution technologies that has been used in many fields, including health. Social media has been used to share health information, deliver behavior change interventions, and monitor symptoms of diseases [19]. In Iran, there has been an increasing use of social media. It has been used as a tool to deliver health education, such as decreasing gingivitis among pregnant women [20]. Thus, there is potential to use social media to deliver oral health education programs.
Telegram is one of the popular used social media platforms in Iran. It is a cloud-based mobile and desktop messaging app that allows countless users to connect, organize, network, and interact easily through various electronic devices. This app has functions superior to other messaging apps. It can send a large volume of files and stickers, serve as a useful and immediate media channel for people sharing images and audio recordings. Telegram could be a useful carrier for education programs in health, communications, social support, and information retrieval [21]. It can be a tool to deliver health education programs [22]. Through Telegram, people can receive information from various sources, which could help to increase health behavior [23]. The results of a study by ISPA (Iranian Student Opinion Polling Center in Jahade Deneshgahi University) showed that in March 2016, 71% of Iranian youth used Telegram, and 49% used Instagram [24]. Also, after its filtering by the government, about 80% of Telegram users in Iran did not leave Telegram [25].
Oral self-care behaviors are not satisfactory among students, the incidence of gingivitis is high in them and training programs have slightly improved their gingivitis. This study aimed to evaluate a Telegram delivered oral health education program on the gingival index, perceived benefits, perceived barriers, self-efficacy, and motivational beliefs regarding DCB in Iranian students with gingivitis.
Methods
This randomized controlled trial was conducted in Sanandaj city, Iran, from January to December 2019. Two-stage random sampling was used. Eight secondary schools (4 female and four male schools) were selected by simple random sampling from 1499 schools in two Regions of Sanandaj. 350 students of the four schools selected (two female and two male schools). In the second stage of the sampling process, 80 participants who met the inclusion criteria were randomly selected from each school and divided into the intervention and control groups (Twenty students were selected from each school by random sampling method and randomly divided into the intervention and control groups, yielding a total of 160 participants). The inclusion criterion for the schools was using of telegram apps to educate students. Participants' inclusion criteria were age ranged from 12 to 19, lack of dental cleaning tools such as toothbrush and dental floss (via self-report), being in pre-contemplation and contemplation stages of DCB, presence of gingivitis (inflammation of the gums as assessed by a dentist in a classroom, and having access to Telegram app by mobile of their parents. The exclusion criteria were students with fixed orthodontics.
The participants' demographic variables were collected (gender, parents' education, parents' job, oral Health assessment and the number of referrals to dentist). A questionnaire was used, which contained the following components:
-Constructs of the trans-theoretical model: The constructs of the trans-theoretical model included self-efficacy (10 items with 4-point Likert scale, cut-off point of 20 (average score), reliability of 0.85, and content validity of 0.81); perceived barriers (10 items with 5-point Likert scale, cut-off point of 25 (average score), reliability of 0.81, and validity of 0.83); and perceived benefits (8 items with 4-point Likert scale, cut-off point of 20 (average score), reliability of 0.85, and validity of 0.84). The questionnaire used in our study has previously been published [15].
-DCB: There were four items to assess DCB (an instrument.). The Kappa coefficients of 4 DCB items were 0.75 in the first stage, 0.78 in the second stage, 0.45, and 0.75 in the third and fourth stages, respectively [17, 26]. Table 1 presents how students were placed in each stage of DCB.
-Motivational beliefs: Motivational beliefs included five items with a 5-point Likert scale, the cut-off point of 12.5 (average score), reliability of 0.82, and validity of 0.84. The items of motivational beliefs were formulated based on the perspective and experience of students grounded in a previous qualitative study [27]. Its reliability and validity had been confirmed [18].
-Gingival index (GI): It was recorded by a dentist who assessed the students in the classroom. This index has three degrees, including degree 1: Partial change in gingival color and tissue (Low score), degree 2: Gingival redness, edema and gingival restoration and degree (average score), degree 3: severe inflammation and a gingival ulcer (high score) [1, 28].
This study was obtained approval from the Iranshahr University of Medical Sciences and Kurdistan University of Medical Sciences. The objectives and research method were explained to the authorities (school principals and heads of educational organizations), parents, and students. Written informed consent was taken from students and their parents. Participation in the study was voluntary, and confidentiality of data was emphasized. Also, this study adheres to CONSORT guidelines and includes a completed CONSORT checklist. Based on the trans-theoretical model, interventional strategies were developed for students in the pre-contemplation stage of DCB (Consciousness Raising, Dramatic Relief, Environmental Reevaluation, and Self-Liberation). The intervention aimed to increase students' perceived benefits, self-efficacy, DCB and reduce perceived barriers and gingivitis. Bandura's strategies were employed in the intervention, including setting simple and definite educational objectives, encouraging oral health practices, reframing obstacles, or replacing them with positive interventions [29]. The advantages of having good oral health (fresh breath, prevention of gingivitis and cardiovascular diseases, etc.) were delivered through a Telegram channel to increase perceived benefits.
Bass's tooth brushing technique was presented as a simple and efficient method through ten educational clips to teach tooth brushing [30] and correct use of dental floss and toothpick. The training program included motivational beliefs (such as dental cleaning to mean appreciating God) in DCB were part of the training program. The intervention was performed three times a week over three consecutive weeks (Table 2). Each time images of the oral cavity and healthy and inflammatory gum, materials about the benefits of behavior, motivational beliefs related to dental health, self-efficacy, and overcoming obstacles were sent to the Telegram channel. During the transmission of the educational content, the researchers ensured that the participants observed and read the messages (in-app Telegram when a delivered message was read, it could be tracked). The researchers went to selected schools, informed participants how much time it would take to complete the questionnaire, and impressed upon them that they should be honest. The questionnaires were anonymous and took 12-15 minutes to complete; it was administered at baseline and 24 weeks after the intervention was delivered.
Oral health is a state of tooth structure and tissue linked to physical, psychological, and social well-being. Oral health co-determines if and how people will be able to talk, eat and socialize [1-3]. Despite the importance of oral health, more than 99% of people worldwide suffer from oral diseases [4], negatively impacting their communication abilities, daily performance, and poor voice quality. They may also suffer from pain and anxiety [5-7]. Worldwide, dental caries has increased significantly, especially in adolescents [8]. The World Health Organization (WHO) has called for global initiatives to reduce the burden of oral diseases in adolescents [9].
Located in the eastern Mediterranean region [10], Iran is one of the youngest countries in the world which 50% are under the age of 30 years [11]. The incidence of dental caries in Iranian students is over 90% [12], and one-third of them suffer from gingivitis [13]. These figures indicated the necessity of educational programs which aim to maintain and promote oral health in students [14, 15].
Many education programs developed based on behavioral change models, such as the trans-theoretical model, have shown high efficacy in preventing oral diseases [1]. Although some studies have evaluated the application of the trans-theoretical model in promoting Dental Cleaning Behavior (DCB) [1, 16, 17], the researchers did not have access to research that assessed the effects of a health education program supported by the trans-theoretical model and delivered via social media app.
The Trans-Theoretical Model (TTM) is a purposeful behavioral change model. It is a systematic study of individuals' behavioral changes and describes how people move dynamically through five different stages of behavioral changes. The four core constructs of TTM are stages of change (Precontemplation, Contemplation, Preparation, Action, Maintenance), self-efficacy, decisional balance, and change processes. The TTM holds that people begin to perceive more benefits than disadvantages from adopting positive behavior changes as they move through the later stages [18].
Social media is one of the recent revolution technologies that has been used in many fields, including health. Social media has been used to share health information, deliver behavior change interventions, and monitor symptoms of diseases [19]. In Iran, there has been an increasing use of social media. It has been used as a tool to deliver health education, such as decreasing gingivitis among pregnant women [20]. Thus, there is potential to use social media to deliver oral health education programs.
Telegram is one of the popular used social media platforms in Iran. It is a cloud-based mobile and desktop messaging app that allows countless users to connect, organize, network, and interact easily through various electronic devices. This app has functions superior to other messaging apps. It can send a large volume of files and stickers, serve as a useful and immediate media channel for people sharing images and audio recordings. Telegram could be a useful carrier for education programs in health, communications, social support, and information retrieval [21]. It can be a tool to deliver health education programs [22]. Through Telegram, people can receive information from various sources, which could help to increase health behavior [23]. The results of a study by ISPA (Iranian Student Opinion Polling Center in Jahade Deneshgahi University) showed that in March 2016, 71% of Iranian youth used Telegram, and 49% used Instagram [24]. Also, after its filtering by the government, about 80% of Telegram users in Iran did not leave Telegram [25].
Oral self-care behaviors are not satisfactory among students, the incidence of gingivitis is high in them and training programs have slightly improved their gingivitis. This study aimed to evaluate a Telegram delivered oral health education program on the gingival index, perceived benefits, perceived barriers, self-efficacy, and motivational beliefs regarding DCB in Iranian students with gingivitis.
Methods
This randomized controlled trial was conducted in Sanandaj city, Iran, from January to December 2019. Two-stage random sampling was used. Eight secondary schools (4 female and four male schools) were selected by simple random sampling from 1499 schools in two Regions of Sanandaj. 350 students of the four schools selected (two female and two male schools). In the second stage of the sampling process, 80 participants who met the inclusion criteria were randomly selected from each school and divided into the intervention and control groups (Twenty students were selected from each school by random sampling method and randomly divided into the intervention and control groups, yielding a total of 160 participants). The inclusion criterion for the schools was using of telegram apps to educate students. Participants' inclusion criteria were age ranged from 12 to 19, lack of dental cleaning tools such as toothbrush and dental floss (via self-report), being in pre-contemplation and contemplation stages of DCB, presence of gingivitis (inflammation of the gums as assessed by a dentist in a classroom, and having access to Telegram app by mobile of their parents. The exclusion criteria were students with fixed orthodontics.
The participants' demographic variables were collected (gender, parents' education, parents' job, oral Health assessment and the number of referrals to dentist). A questionnaire was used, which contained the following components:
-Constructs of the trans-theoretical model: The constructs of the trans-theoretical model included self-efficacy (10 items with 4-point Likert scale, cut-off point of 20 (average score), reliability of 0.85, and content validity of 0.81); perceived barriers (10 items with 5-point Likert scale, cut-off point of 25 (average score), reliability of 0.81, and validity of 0.83); and perceived benefits (8 items with 4-point Likert scale, cut-off point of 20 (average score), reliability of 0.85, and validity of 0.84). The questionnaire used in our study has previously been published [15].
-DCB: There were four items to assess DCB (an instrument.). The Kappa coefficients of 4 DCB items were 0.75 in the first stage, 0.78 in the second stage, 0.45, and 0.75 in the third and fourth stages, respectively [17, 26]. Table 1 presents how students were placed in each stage of DCB.
-Motivational beliefs: Motivational beliefs included five items with a 5-point Likert scale, the cut-off point of 12.5 (average score), reliability of 0.82, and validity of 0.84. The items of motivational beliefs were formulated based on the perspective and experience of students grounded in a previous qualitative study [27]. Its reliability and validity had been confirmed [18].
-Gingival index (GI): It was recorded by a dentist who assessed the students in the classroom. This index has three degrees, including degree 1: Partial change in gingival color and tissue (Low score), degree 2: Gingival redness, edema and gingival restoration and degree (average score), degree 3: severe inflammation and a gingival ulcer (high score) [1, 28].
This study was obtained approval from the Iranshahr University of Medical Sciences and Kurdistan University of Medical Sciences. The objectives and research method were explained to the authorities (school principals and heads of educational organizations), parents, and students. Written informed consent was taken from students and their parents. Participation in the study was voluntary, and confidentiality of data was emphasized. Also, this study adheres to CONSORT guidelines and includes a completed CONSORT checklist. Based on the trans-theoretical model, interventional strategies were developed for students in the pre-contemplation stage of DCB (Consciousness Raising, Dramatic Relief, Environmental Reevaluation, and Self-Liberation). The intervention aimed to increase students' perceived benefits, self-efficacy, DCB and reduce perceived barriers and gingivitis. Bandura's strategies were employed in the intervention, including setting simple and definite educational objectives, encouraging oral health practices, reframing obstacles, or replacing them with positive interventions [29]. The advantages of having good oral health (fresh breath, prevention of gingivitis and cardiovascular diseases, etc.) were delivered through a Telegram channel to increase perceived benefits.
Bass's tooth brushing technique was presented as a simple and efficient method through ten educational clips to teach tooth brushing [30] and correct use of dental floss and toothpick. The training program included motivational beliefs (such as dental cleaning to mean appreciating God) in DCB were part of the training program. The intervention was performed three times a week over three consecutive weeks (Table 2). Each time images of the oral cavity and healthy and inflammatory gum, materials about the benefits of behavior, motivational beliefs related to dental health, self-efficacy, and overcoming obstacles were sent to the Telegram channel. During the transmission of the educational content, the researchers ensured that the participants observed and read the messages (in-app Telegram when a delivered message was read, it could be tracked). The researchers went to selected schools, informed participants how much time it would take to complete the questionnaire, and impressed upon them that they should be honest. The questionnaires were anonymous and took 12-15 minutes to complete; it was administered at baseline and 24 weeks after the intervention was delivered.
Table 1) Key for determining the stage of change based on responses to the stages of change instrument [17]

Table 2) Content of 3 weeks of intervention based on trans-theoretical model

SPSS 21 software and Telegram TALAEE (unknown version) application were used. Data were analyzed using the Chi-square test (to examine the number of demographics variables in two groups, also for distribution of stages of change of interdental cleaning behavior in the two studied groups), independent t-test (to assess study’s variables after intervention), and paired t-test ( to assess study’s variables after and before of intervention).
Findings
In this study, 160 male and female students with a mean age of 14.87±2.26 (range from 12 to 18 years) were included in two intervention and control groups. The mean scores of motivational beliefs, perceived benefits, and perceived self-efficacy were low, and those of perceived barriers and GI were high. There was no significant difference between the two groups in baseline measures (p>0.05).
There was no statistically significant difference between the demographic characteristics in the two groups (p>0.05). The majority of students had never visited a dentist for dental examination and reported a good oral health evaluation (Table 3).
The distribution of stages of DCB in both groups after the intervention was shown in Diagram 1. The results of chi-square indicated a significant difference between intervention and control groups in DCB. Further, 71.3% (n=57) of students in the intervention group (versus 10.1% (n=10) in control group) performed the DCB (χ2=59.79; df=4; p<0.01), i.e. they were either in the action or maintenance stage.
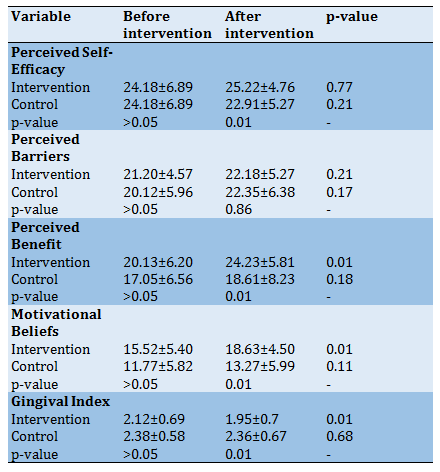
Comparison of mean scores of perceived self-efficacy, benefits and barriers, motivational beliefs, and gingival index between intervention and control groups before and after intervention shown in Table 4. The paired t-test showed an increase in the mean scores of perceived benefits and motivational beliefs in the intervention group and a decrease in GI (p<0.05) at follow-up. There were significant differences between intervention and control groups in the mean scores of perceived self-efficacy (p=0.01), perceived benefits (p=0.01), motivational beliefs (p=0.01), and gingival index (p=0.01) after intervention (Table 4).
Table 3) Frequency of characteristics of the studied students
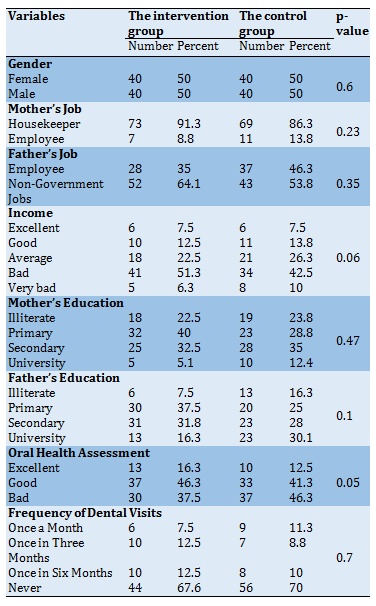
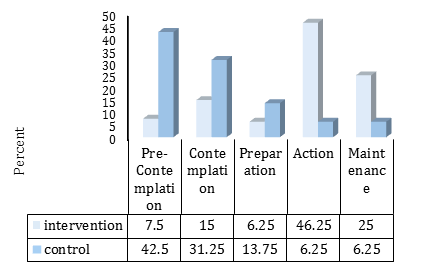
Diagram 1) Distribution of stages of change of interdental cleaning behavior in the two studied groups 24 weeks after the intervention
Findings
In this study, 160 male and female students with a mean age of 14.87±2.26 (range from 12 to 18 years) were included in two intervention and control groups. The mean scores of motivational beliefs, perceived benefits, and perceived self-efficacy were low, and those of perceived barriers and GI were high. There was no significant difference between the two groups in baseline measures (p>0.05).
There was no statistically significant difference between the demographic characteristics in the two groups (p>0.05). The majority of students had never visited a dentist for dental examination and reported a good oral health evaluation (Table 3).
The distribution of stages of DCB in both groups after the intervention was shown in Diagram 1. The results of chi-square indicated a significant difference between intervention and control groups in DCB. Further, 71.3% (n=57) of students in the intervention group (versus 10.1% (n=10) in control group) performed the DCB (χ2=59.79; df=4; p<0.01), i.e. they were either in the action or maintenance stage.
Comparison of mean scores of perceived self-efficacy, benefits and barriers, motivational beliefs, and gingival index between intervention and control groups before and after intervention shown in Table 4. The paired t-test showed an increase in the mean scores of perceived benefits and motivational beliefs in the intervention group and a decrease in GI (p<0.05) at follow-up. There were significant differences between intervention and control groups in the mean scores of perceived self-efficacy (p=0.01), perceived benefits (p=0.01), motivational beliefs (p=0.01), and gingival index (p=0.01) after intervention (Table 4).
Table 3) Frequency of characteristics of the studied students


Diagram 1) Distribution of stages of change of interdental cleaning behavior in the two studied groups 24 weeks after the intervention
Table 4) Comparison of mean±SD of outcomes in the intervention and control groups before and after the edu
Discussion
The present study delivered an oral health education program to Iranian students via social media Telegram. In the abovementioned studies, the researchers used audio-visual media, lectures, and meetings to promote DCB. In our study, the majority of students in the intervention group performed the DCB. The media through which the intervention was delivered may have been of particular importance. The Telegram channel enables a new experience of communication and training, easy and rapid access to updated information, diverse and appealing educational content, adequate social support (informational support), and increased perceived benefits of the behavior. It should be noted that knowledge and understanding of health and illnesses will be improved via social networks [31], which is in line with the fundamentals of the health belief model, stating that doing the behavior will be increased if the perceived benefits of the behavior are enhanced [16, 32]. However, whether a messaging app delivered intervention is superior to an intervention that relies on more traditional means of health education needs to be addressed by future studies which include both interventions.
The findings showed that 70% of students in the intervention group were in the final stages of DCB after the training program and used dental cleaning tools, indicating a significant difference between intervention and control groups. Our results agreed with the study of Rahmani et al. After the intervention, 67.5% of pregnant women in the intervention group (versus 16.6% in the control group) performed the dental cleaning behavior [20].
After the intervention, the results revealed a statistically significant difference between intervention and control groups in the mean scores of perceived self-efficacy, perceived benefits, motivational beliefs, and GI, but not in the mean score of perceived barriers. In line with our findings, Damle et al. reported that the interventional program in improving oral hygiene status presented through educational graphs and models reduced the mean GI in the intervention group [33]. de Bate et al. found that web-based training programs improved oral health providers' self-efficacy, awareness, and attitude. The participants in this study asserted that these web-based pieces of training provided more information than other methods and were satisfactory and effective with regard to the patients' evaluation, referral, and treatment [29]. Tavakoli & Fallahi showed that the mean scores of perceived benefits and self-efficacy increased after presenting the training program through lecture and practice [34]. That students' perceived self-efficacy, perceived benefits, motivational beliefs, and GI were significant after intervention might be because we proceeded to improve the students' skills and commitment, control conditions, and encourage them regularly in our training program. According to the planned behavior theory principles, higher self-efficacy and perceived control go hand in hand with higher performance of the behavior [29, 35]. In this regard, a study stated that visual media was more helpful than other educational methods in training the audience and patients [37], which could affect learning and self-efficacy. Other reasons for the significance level of DCB variables in students can be attributed to holding motivational meetings and counseling, especially motivational beliefs to perform the behavior. It is necessary to pay attention to the abovementioned points in web-based health education programs. Although education via social networks is diverse and accessible [23] and increases the individuals' knowledge and skills [29], it does not practically overcome barriers such as fatigue. As for the oral health-related educational programs, it is better to simultaneously use the virtual world (e.g., video) and real world (e.g. social support) and consider the negative consequences of extreme use of these networks by young people.
The use of social media to provide health education can reach a wider range of audiences, which might minimize educational inequalities such as qualified and experienced educators and books. The use of social media to deliver oral health programs might be cheaper in the long run when compared to face-to-face in-person delivery. Social media can also be used in some capacity which there are significant limitations in the implementation of face-to-face public awareness campaigns and educational programs such as infectious diseases outbreaks (like COVID-19 pandemic).
The study was conducted on secondary school students within one region of Iran only. The sample size might be inadequate for the present investigation. The study did not include feedback from users-students, and short-term follow-up was at six months only. Future multi-center trials which are full-powered should be conducted to provide more conclusive evidence on the effects of using social media to deliver oral health interventions. The results of this study can be helpful to the dentists, health professionals, healthcare providers, teachers, and health trainers in schools in designing educational programs for the promotion of oral health. Future studies are recommended to evaluate the efficacy of the oral health education programs delivered via social media in different regions and population groups in Iran. Future studies could also compare the effects of using social media and traditional face-to-face in delivering oral health education programs. Future studies could also include process evaluation to obtain feedback about the intervention from students.
Conclusion
The oral health education intervention via social media in secondary school students could enhance students' oral health. Also, social media platforms have the potential to increase perceived self-efficacy, motivational beliefs, and dental cleaning behavior among students and provide preliminary evidence supporting an oral health program delivered by social media could improve students' DCB, GI, and self-efficacy.
Acknowledgments: -
Ethical Permissions: The current study (research no: 9513-6 and ethical code: IR.IRSHUMS.REC. 1395.6) was approved by the deputy of research and technology at Iranshahr University of Medical Sciences and Kurdistan University of Medical Sciences (research no: IR.MUK.REC.1395/183).
Conflicts of Interests: The authors have no conflict of interest to declare
Authors’ Contribution: Zareban I. (First Author), Main Researcher/Statistical Analyst (15%); Rahmani A. (Second Author), Introduction Writer/Methodologist (10%); Allahqoli L. (Third Author), Discussion Writer (10%); Ghanei Gheshlagh R. (Fourth Author), Discussion Writer (10%); Hashemian M. (Fifth Author), Introduction Writer/Methodologist/Assistant Researcher/Statistical Analyst (15%); Khayyati F. (Sixth Author), Introduction Writer/Methodologist (10%); Wai-chi Chan S. (Seventh Author), Introduction Writer/Methodologist (10%); Volken T. (Eighth Author) Assistant Researcher/Statistical Analyst (10%); Nemat B. (Ninth Author) Methodologist (10%).
Funding/Support: This study was supported by Iranshahr University of Medical Sciences and Kurdistan University of Medical Sciences.

Discussion
The present study delivered an oral health education program to Iranian students via social media Telegram. In the abovementioned studies, the researchers used audio-visual media, lectures, and meetings to promote DCB. In our study, the majority of students in the intervention group performed the DCB. The media through which the intervention was delivered may have been of particular importance. The Telegram channel enables a new experience of communication and training, easy and rapid access to updated information, diverse and appealing educational content, adequate social support (informational support), and increased perceived benefits of the behavior. It should be noted that knowledge and understanding of health and illnesses will be improved via social networks [31], which is in line with the fundamentals of the health belief model, stating that doing the behavior will be increased if the perceived benefits of the behavior are enhanced [16, 32]. However, whether a messaging app delivered intervention is superior to an intervention that relies on more traditional means of health education needs to be addressed by future studies which include both interventions.
The findings showed that 70% of students in the intervention group were in the final stages of DCB after the training program and used dental cleaning tools, indicating a significant difference between intervention and control groups. Our results agreed with the study of Rahmani et al. After the intervention, 67.5% of pregnant women in the intervention group (versus 16.6% in the control group) performed the dental cleaning behavior [20].
After the intervention, the results revealed a statistically significant difference between intervention and control groups in the mean scores of perceived self-efficacy, perceived benefits, motivational beliefs, and GI, but not in the mean score of perceived barriers. In line with our findings, Damle et al. reported that the interventional program in improving oral hygiene status presented through educational graphs and models reduced the mean GI in the intervention group [33]. de Bate et al. found that web-based training programs improved oral health providers' self-efficacy, awareness, and attitude. The participants in this study asserted that these web-based pieces of training provided more information than other methods and were satisfactory and effective with regard to the patients' evaluation, referral, and treatment [29]. Tavakoli & Fallahi showed that the mean scores of perceived benefits and self-efficacy increased after presenting the training program through lecture and practice [34]. That students' perceived self-efficacy, perceived benefits, motivational beliefs, and GI were significant after intervention might be because we proceeded to improve the students' skills and commitment, control conditions, and encourage them regularly in our training program. According to the planned behavior theory principles, higher self-efficacy and perceived control go hand in hand with higher performance of the behavior [29, 35]. In this regard, a study stated that visual media was more helpful than other educational methods in training the audience and patients [37], which could affect learning and self-efficacy. Other reasons for the significance level of DCB variables in students can be attributed to holding motivational meetings and counseling, especially motivational beliefs to perform the behavior. It is necessary to pay attention to the abovementioned points in web-based health education programs. Although education via social networks is diverse and accessible [23] and increases the individuals' knowledge and skills [29], it does not practically overcome barriers such as fatigue. As for the oral health-related educational programs, it is better to simultaneously use the virtual world (e.g., video) and real world (e.g. social support) and consider the negative consequences of extreme use of these networks by young people.
The use of social media to provide health education can reach a wider range of audiences, which might minimize educational inequalities such as qualified and experienced educators and books. The use of social media to deliver oral health programs might be cheaper in the long run when compared to face-to-face in-person delivery. Social media can also be used in some capacity which there are significant limitations in the implementation of face-to-face public awareness campaigns and educational programs such as infectious diseases outbreaks (like COVID-19 pandemic).
The study was conducted on secondary school students within one region of Iran only. The sample size might be inadequate for the present investigation. The study did not include feedback from users-students, and short-term follow-up was at six months only. Future multi-center trials which are full-powered should be conducted to provide more conclusive evidence on the effects of using social media to deliver oral health interventions. The results of this study can be helpful to the dentists, health professionals, healthcare providers, teachers, and health trainers in schools in designing educational programs for the promotion of oral health. Future studies are recommended to evaluate the efficacy of the oral health education programs delivered via social media in different regions and population groups in Iran. Future studies could also compare the effects of using social media and traditional face-to-face in delivering oral health education programs. Future studies could also include process evaluation to obtain feedback about the intervention from students.
Conclusion
The oral health education intervention via social media in secondary school students could enhance students' oral health. Also, social media platforms have the potential to increase perceived self-efficacy, motivational beliefs, and dental cleaning behavior among students and provide preliminary evidence supporting an oral health program delivered by social media could improve students' DCB, GI, and self-efficacy.
Acknowledgments: -
Ethical Permissions: The current study (research no: 9513-6 and ethical code: IR.IRSHUMS.REC. 1395.6) was approved by the deputy of research and technology at Iranshahr University of Medical Sciences and Kurdistan University of Medical Sciences (research no: IR.MUK.REC.1395/183).
Conflicts of Interests: The authors have no conflict of interest to declare
Authors’ Contribution: Zareban I. (First Author), Main Researcher/Statistical Analyst (15%); Rahmani A. (Second Author), Introduction Writer/Methodologist (10%); Allahqoli L. (Third Author), Discussion Writer (10%); Ghanei Gheshlagh R. (Fourth Author), Discussion Writer (10%); Hashemian M. (Fifth Author), Introduction Writer/Methodologist/Assistant Researcher/Statistical Analyst (15%); Khayyati F. (Sixth Author), Introduction Writer/Methodologist (10%); Wai-chi Chan S. (Seventh Author), Introduction Writer/Methodologist (10%); Volken T. (Eighth Author) Assistant Researcher/Statistical Analyst (10%); Nemat B. (Ninth Author) Methodologist (10%).
Funding/Support: This study was supported by Iranshahr University of Medical Sciences and Kurdistan University of Medical Sciences.
Article Type: Original Research |
Subject:
Health Promotion Approaches
Received: 2021/02/14 | Accepted: 2021/06/26 | Published: 2022/01/24
Received: 2021/02/14 | Accepted: 2021/06/26 | Published: 2022/01/24
References
1. Hashemian M, Fallahi A, Tavakoli G, Zarezadeh Y, Nemat Shahr Babaki B, Rahaei Z. Study of the impact of education on inter-dental cleaning behavior based on trans-theoretical model. Oral Health Prev Dent. 2012;10(1):37-46. [Link]
2. Morowatisharifabad M, Fallahi A, Nadrian H, Haerian A, Nemat Babaki B. Interdental cleaning behaviour and its relationship with psychological constructs based on the trans-theoretical model. Oral Health Prev Dent. 2011;9(3):211-20. [Link]
3. Rostami S, Fallahi A, Pashaei T, Roshani D. Association of trans-theoretical model (TTM) based exercise behavior change with body image evaluation among female Iranian students. Int J Pediatr. 2017;5(3):4613-23. [Persian] [Link]
4. Tahani B, Moosavi SP. Assessment of oral health status and health behaviors in the adult population of nomadic tribes (2016). J Mashhad Dent Sch. 2018;42(4):307-19. [Persian] [Link]
5. Ortiz-Barrios LB, Granados-Garcia V, Cruz-Hervert P, Moreno-Tamayo K, Heredia-Ponce E, Sanchez-Garcia S. The impact of poor oral health on the oral health-related quality of life (OHRQoL) in older adults: The oral health status through a latent class analysis. BMC Oral Health. 2019;19(1):141. [Link] [DOI:10.1186/s12903-019-0840-3] [PMID] [PMCID]
6. Nemat-Shahrbabaki B, Fallahi A, Valiee S, Zarei M, Fallahi P. Exploring self-care needs of pregnant women with gingivitis: A qualitative study in Iran. Iran J Nurs Midwifery Res. 2018;23(4):292-7. [Link] [DOI:10.4103/ijnmr.IJNMR_163_17] [PMID] [PMCID]
7. Shahrbabaki B, Hashemian M, Fallahi A, Rahmani A, Saedpanah A. The relationship between stages of dental cleaning behavior change based on trans-theoretical Model (TTM) with school role and social support in students. Int J Pediatr. 2017;5(5):4939-49. [Persian] [Link]
8. Moynihan P, Petersen PE. Diet, nutrition and the prevention of dental diseases. Public Health Nutr. 2004;7(1):201-26. [Link] [DOI:10.1079/PHN2003589] [PMID]
9. Hobdell M, Petersen PE, Clarkson J, Johnson N. Global goals for oral health 2020. Int Dent J. 2003;53(5):285-8. [Link] [DOI:10.1111/j.1875-595X.2003.tb00761.x] [PMID]
10. Petersen PE, Bourgeois D, Ogawa H, Estupinan-Day S, Ndiaye C. The global burden of oral diseases and risks to oral health. Bull World Health Organ. 2005;83(9):661-9. [Link]
11. amar.org.ir [Internet]. Tehran: Statistical Center of Iran; 2017 [Unknown cited]. Available from: https://www.amar.org.ir/news/ID/2566/. [Persian] [Link]
12. Esmaeilzadeh S, Abbasi A, Nikniaz S, Fathi B, Saeli E. Evaluation of Oral and Dental Health among 12 Year-Old Students in Jolfa, East Azerbaijan. Depict Health. 2017;7(4):30-6. [Persian] [Link]
13. Gharibi F, Asghari-Jafarabadi M, Amini Daghalian B. Survey oral health status and its effective factors among primary school boy students of Paveh city via DMFT, CF and gingivitis indicators in 2013. Depict Health. 2014;5(3):5-12. [Persian] [Link]
14. Fallahi A, Ghofranipour F, Ahmadi F, Malekafzali B, Hajizadeh E. Challenges of Iranian adolescents for preventing of dental caries. Iran Red Crescent Med J. 2014;16(9):15009. [Link] [DOI:10.5812/ircmj.15009] [PMID] [PMCID]
15. Shirzad M, Taghdisi MH, Dehdari T, Abolghasemi J. Oral health education program among pre-school children: an application of health-promoting schools approach. Health Promot Perspect. 2016;6(3):164-170. [Link] [DOI:10.15171/hpp.2016.26] [PMID] [PMCID]
16. Solhi M, Shojaei Zadeh D, Seraj B, Faghih Zadeh S. The application of the health belief model in oral health education. Iran J Public Health. 2010;39(4):114-9. [Link]
17. Tilliss T, Stach D, Cross-Poline G, Annan S, Astroth D, Wolfe P. The Transtheoretical model applied to an oral self-care behavioral change: Development and testing of instruments for stages of change and decisional balance. J Dent Hyg. 2003;77(1):16-25. [Link]
18. Liu K, Kueh Y, Arifin W, Kim Y, Kuan G. Application of trans-theoretical model on behavioral changes, and amount of physical activity among university's students. Front Psychol. 2018;9:2402. [Link] [DOI:10.3389/fpsyg.2018.02402] [PMID] [PMCID]
19. Kapoor KK, Tamilmani K, Rana N, Patil P, Dwivedi YK, Nerur S. Advances in social media research: Past, present and future. Inf Syst Front. 2018;20:531-58 [Link] [DOI:10.1007/s10796-017-9810-y]
20. Rahmani A, Allahqoli L, Hashemian M, Ghanei Gheshlagh R, Nemat-Shahrbabaki B. Effect education based on trans-theoretical model on reduction of the prevalence of gingivitis among pregnant women: Application of Telegram social network. Sci J Kurdistan Univ Med Sci. 2019;24(2):74-83. [Persian] [Link] [DOI:10.29252/sjku.24.2.74]
21. Rezaei M, Shobeiri S, Sarmadi M, Larijani M. The effect of Instagram social network usage on the promotion of environmental Literacy of students. Environ Sci. 2016;14(3):89-106. [Persian] [Link]
22. Balappanavar A, Sardana V, Hegde P. Social networking and oral health education. Int J Sci Stud. 2013;1(1):16-9. [Link]
23. Bull SS, Breslin LT, Wright EE, Black SR, Levine D, Santelli JS. Case study: An ethics case study of HIV prevention research on Facebook: The just/us study. J Pediatr Psychol. 2011;36(10):1082-92. [Link] [DOI:10.1093/jpepsy/jsq126] [PMID] [PMCID]
24. Iranian students new agency. Telegram and Instagram use among adolescences [Internet]. Tehran: Iranian students New Agency; 2019 [Unknown cited]. Available from: https://www.isna.ir/news/98020301268. [Persian] [Link]
25. Iranian students polling agency. Poll about using Telegram [Internet]. Tehran: Iranian Students Polling Agency; 2018 [Unknown cited]. Available from: Not Found. [Link]
26. Taymoori P, Fallahi A, Berry T. Developing an instrument to measure dental flossing in Iranian adolescents. East J Med. 2011;16(4):261-8. [Link]
27. Fallahi A, Ghofranipour F, Ahmadi F, Hajizadeh E, Malekafzali B. Psychometric properties of questionnaire of predicting factors for dental caries in adolescents: Fitness theory through factor analysis. J Sabzevar Univ Med Sci. 2014;21(1):69-80. [Persian] [Link]
28. Rocha MO, Oliveira DD, Costa FO, Pires LR, Diniz AR, Soares RV. Plaque index and gingival index during rapid maxillary expansion of patients with unilateral cleft lip and palate. Dent Press J Orthod. 2017;22(6):43-8. [Link] [DOI:10.1590/2177-6709.22.6.043-048.oar] [PMID] [PMCID]
29. Debate RD, Severson H, Zwald ML, Shaw T, Christiansen S, Koerber A, et al. Development and evaluation of a web-based training program for oral health care providers on secondary prevention of eating disorders. J Dent Educ. 2009;73(6):718-29. [Link] [DOI:10.1002/j.0022-0337.2009.73.6.tb04751.x]
30. Bhardwaj VK, Sharma KR, Luthra RP, Jhingta P, Sharma D, Justa A. Impact of school-based oral health education program on oral health of 12 and 15 years old school children. J Edu Health Promot. 2013;2:33. [Link] [DOI:10.4103/2277-9531.115820] [PMID] [PMCID]
31. Chou WS, Hunt YM, Beckjord EB, Moser RP, Hesse BW. Social media use in the United States: Implications for health communication. J Med Internet Res. 2009;11(4):48. [Link] [DOI:10.2196/jmir.1249] [PMID]
32. Fallahi A, Shahrbabaki B, Hashemian M, Kahanali A. The needs of women referring to health care centers for doing pap smear test. Iran J Obstet Gynecol Infertil. 2016;19(6):1-10. [Persian] [Link]
33. Damle SG, Patil A, Jain S, Damle D, Chopal N. Effectiveness of supervised toothbrushing and oral health education in improving oral hygiene status and practices of urban and rural school children: A comparative study. J Int Soc Prev Community Dent. 2014;4(3):175-81. [Link] [DOI:10.4103/2231-0762.142021] [PMID] [PMCID]
34. Tavakoli G, Fallahi A. The effect of educating mothers in inter-dental cleaning behavior on their children's dental health behavior: Testing the trans-theoretical model. Health Educ Health Promot. 2013;1(2):5-19. [Persian] [Link]
35. Ajzen I. The theory of planned behaviour: Reactions and reflections. Psychol Health. 2011;26(9):1113-27. [Link] [DOI:10.1080/08870446.2011.613995] [PMID]
36. Rahmani A, Hamanajm S, Allahqoli L, Fallahi A. Factors affecting dental cleaning behaviour among pregnant women with gingivitis. Int J Dent Hyg. 2019;17(3):214-20. [Link] [DOI:10.1111/idh.12387] [PMID]
37. Mohamadnejad E, Shariyat E, Bigjani J, Abotalebi G. Oral health status of elementary school students in Saveh, 2009. J Res Dev Nurs Midwifery Gorgan. 2011;8(1):74. [Persian] [Link]
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |





