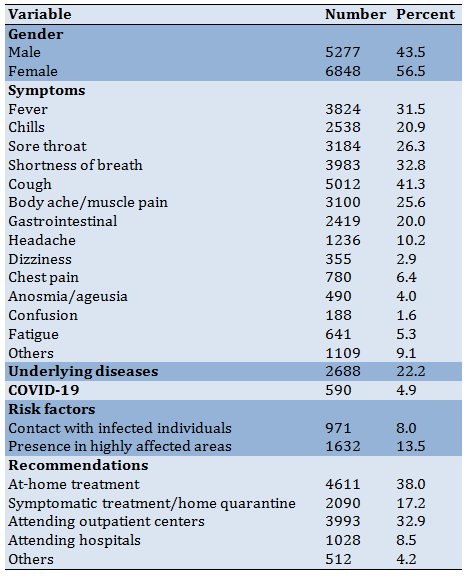
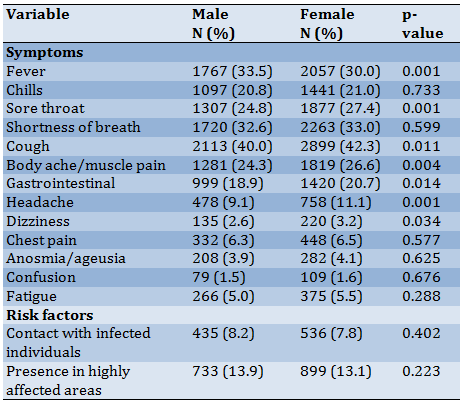
Fallahi,S. , , Hesam,A. , , Arabi,A. , , Shojaee,A. , , Zoghi,G. , , Hesam,M. , , Shahali,Z. , and Ayoubian,A. . "The Self-Report Symptoms of COVID-19 in Iranian Population Through a Teleconsultation-Based Service", Health Education and Health Promotion, 10, 2, 2025, 265-269.